INTRATUMORAL CANCER CHEMOTHERAPY

INTRATUMORAL CANCER CHEMOTHERAPY AND IMMUNOTHERAPY THROUGH A FLEXIBLE BRONCHOSCOPE: A NOVEL THERAPEUTIC CONCEPT IN THE MANAGEMENT OF MALIGNANT AIRWAY OBSTRUCTİON.
Seyhan I. Celikoglu, MD,* Firuz Celikoglu, MD,* and Eugene P. Goldberg, PhD†
DEFINITION
Intratumoral chemotherapy is a novel interventional bronchoscopy technique, which involves injection of cytotoxic drugs directly into the tumoral tissue through a flexible bronchoscope .
Intratumoral chemotherapy deals with the selective destruction of malignant cells through the cytotoxic effects of anticancer drugs but spares normal tissue. In addition to the advantage of initial eradication of tumoral burden inside the obstructed airways, maintenance of weekly intratumoral therapy for 6 to 8 weeks also provides a therapeutic effect of locoregional chemotherapy. Indeed, in newly diagnosed patients, the intratumoral chemotherapy constitutes a neoadjuvant therapy for irradiation or the other conventional cancer treatments.
HISTORICAL BACK GROUND OF INTRATUMORAL INJECTION OF CHEMOTHERAPEUTIC AGENTS
Direct injection of anticancer drugs into the malignant endobronchial tumors has been successfully tested and used by Celikoglu et al. at the Cerrahpasa Medical Faculty of Istanbul University since 1986. In the beginning, the intratumoral chemotherapy was applied mostly for palliation of the bronchial obstruction in patients having relapse after previous conventional cancer treatments. The studies of Goldberg demonstrated that the injected cytotoxic drugs into the tumor also provide a locoregional chemo- or immune therapy in addition to the debulking effect. In view of these studies, since 1998, we are using the intratumoral chemotherapy with cisplatin in patients with newly diagnosed inoperable lung cancer as an adjuvant locoregional chemotherapy before administration of radiotherapy.
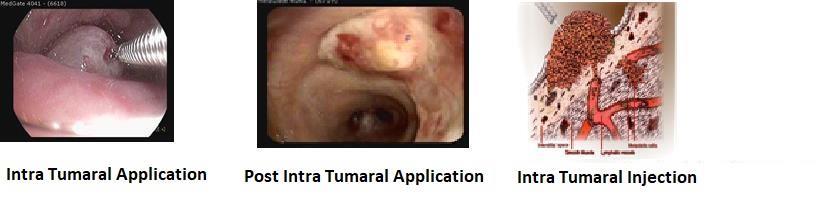
TECHNIQUE AND EQUIPMENT FOR THE INJECTION OF CYTOTOXIC DRUGS THROUGH
A FLEXIBLE BRONCHOSCOPE
Equipment Needs Intratumoral chemotherapy can be performed through flexible bronchoscope under local anesthesia on an out patient basis.
Flexible Bronchoscopy:
Patients undergo routine bronchoscopy with standard monitoring in a fully equipped bronchoscopy suite. Before the bronchoscopy, routine clinical data are obtained, including, coagulation parameters, and routine biochemistry. The chest radiography and computerized axial tomographic (CAT) scan of the chest should be carefully reviewed to locate with precision the extent of the extraluminal localization of the tumor. An intravenous access site is established, and normal saline is infused during the procedure. Monitoring includes an electrocardiogram, noninvasive blood pressure recording, and oxygen saturation. Supplemental oxygen, is administered nasally. Topical anesthesia of the oral–nasopharynx is achieved with 4% lidocaine. Conscious sedation is achieved with intravenous midazolamand meperidine.
What Happens During and After Injecting the Cytotoxic Drug Into the Tumor?
When the tumor is visible through the bronchoscope as an intraluminal exophytic mass, injection of the cytotoxic drug produces the following endoscopically visible effects. While injecting the cytotoxic drug, the surface of the tumor around the needle becomes paler and whiter. This is probably the result of swelling of the tumoral tissue by added volüme of a liquid in a restricted space. Shortly after local administration of the drug, there is a reduction in size of the tumor and accompanying changes, ie, atelectasis or obstructive pneumonia. When tumor infiltrates into the bronchial membrane, the infiltrative tumoral changes improve markedly by the direct injection.
Intratumoral injection of cytotoxic drugs also provides a hemostatic effect on tumor tissue. In general, bleeding on the surface of the tumor stops after injection. The hemostatic effect probably is the result of a vasoconstriction of the small vessels in or around the tumor mass. This could occur because of a reaction of vessels to the very high concentration of cytotoxic drug. Also, the volume of drug solution added by injection in a restricted space could compress the vessels inside the tumor. This could cause an oligemia in the tumor bulk contributing to hemostasis. Intravascular formation of thromboses, which probably occurs after the cytotoxic drug injection, could contribute to the hemostasis as well.
The beneficial debulking effects of intratumoral administration of cytotoxic drug on tumoral tissue presumably ocur as a result of the contact of tumor cells with a very high concentration of anticancer material, which causes an instant necrosis, and consequently the reduction of the tumor volume.
Postoperative Care
Intratumoral chemotherapy does not require any particular immediate follow-up care. Patients treated under local anesthesia and conscious sedation have been sent home on the same day of intervention.
Follow Up
Reexpansion the collapsed area of the lung can be confirmed with a chest x-ray. Nevertheless, we recognize the delayed effect of necrosis from injection of cytotoxic drug and generally do not expect a change in the chest film immediately.
Corticosteroids are not routinely administered and are considered only after treatment of laryngeal and tracheal lesions, in which the risk of an edematous reaction is greatest.
The hemostatic effect of cytotoxic drug injection is often sufficient to stop hemoptysis. Improvement could be delayed and occurs only some hours to a day after intratumoral injection. In some patients with obstruction of the trachea or carina plus of the main bronchi, dyspnea could be worsened 1 to 6hours after the first session of intratumoral injections. This could be the result of reactive edema, accumulation of necrotic tumor cell coagulum, and inspissated secretions. In such patients, dexamethasone is administered intravenously to decrease the reactive edema at the intratumoral injection site.
A cleanup bronchoscopy is performed immediately with removal of necrotic tumor debris and accumulated secretions by piecemeal resection with forceps and suction. This cleaning procedure immediately restores the opening of the airway lumen with the alleviation of dyspnea.
In patients with postobstructive pneumonia at the initial session after debulking, the pus built up beyond the postobstructed airways must be carefully removed by suction. Otherwise, the pus spills out of the healthy airways. The intratumoral necrotic tumor debridement also allows injection of cytotoxic drug more deeply into any residual tumor mass attached to the bronchial wall in mixed tumors.
Schedule of the Intratumoral Chemotherapy Sessions (Cycles)
In newly diagnosed inoperable cases, direct injections are carried out weekly for 3 weeks (days 1, 8, 15, and 21). Thereafter, radiotherapy is started. If a tumor occludes the airway in a patient relapsing after conventional cancer treatments, maintenance intratumoral chemotherapy continues weekly for 6 to 8 weeks or more (days 1, 8, 15, 22, and so on). If the obstruction is relieved and the bronchial lumen remains open, bronchoscopy controls should be repeated monthly for 4 to 6 months and then 3 monthly for 1 year.
THE EFFICIENCY AND PLACE OF INTRATUMORAL CHEMOTHERAPY AMONG THE OTHER INTERVENTIONAL BRONCHOSCOPIC PROCEDURES
In recent clinical studies, systemic administration of cytotoxic drugs before radiotherapy have been used extensively as neoadjuvant chemotherapy with improvement of survival.
As a consequence, safer and more aggressive (higher-dose) administration of toxic chemotherapy or immunotherapy directly to a tumor site, ie, intratumoral therapy, could be considered an attractive alternative to systemic treatment. Indeed, our recent study indicates potentiating or synergistic effect with the combinedtreatment of intratumoral chemotherapy and irradiation. Intratumoral chemotherapy through a flexible bronchoscope can be added concomitantly or any time after conventional lung cancer treatment modalities. It is a novel locoregional chemotherapy procedure and as such should be integrated into the plan of action of treatments for bronchial carcinomas.
CONCLUSION
Intratumoral chemotherapy is a novel therapeutic concept in the management of malignant airway obstruction.
Intratumoral chemotherapy offers an alternative therapy for endobronchial tumor ablation with significant safety as well as being extremely inexpensive.
REFERANCES:
1. Goldberg EP, Hadba HR, Almond BA, et al. Intratumoral cancer chemotherapy
and immunotherapy: opportunities for non-systemic preoperative
drug delivery. J Pharm Pharmacol. 2002;54:159–180.
2. Celikoglu SI, Celikoglu F. Direct injection of several anticancer drugs into endobronchial malignant tumour in the palliation of major airways obstruction [Abstract]. Eur Respir J. 1991;4(suppl 14):303s.
3-Seyhan I. Çelikoğlu, Firuz Çelikoğlu. Direct injection of anti-cancer drugs into endobronchial tumours for palliation of major airway obstruction. Postgrad Med J 1997; 73: 159-162 ©
4. Celikoglu F, Celikoglu SI, . Intratumoral chemotherapy with 5-fluorouracil for palliation of bronchial cancer in patients with severe airway obstruction. J Pharm Pharmacol. 2003;55:1441–1447.
5. Celikoglu F, Celikoglu SI. Initial combination therapy with intratumoral injection of cisplatin and irradiation for inoperable non-small cell lung cancer [Abstract]. Am J Respir Crit Care Med. 2004;169:A334..
6--Seyhan I. Çelikoğlu, Firuz Çelikoğlu, Eugene P. Goldberg. “Endo bronchial intratumoral chemotherapy (EITC) followed by surgery in early non-small cell lung cancer with polypoid growth cousing erroneous impression of advanced disease”.
Lung Cancer .2006;54: 339-346
7-Firuz Çelikoğlu ,Seyhan I. Çelikoğlu, , Amanda M.York, Eugene P.Goldberg “Intratumoral non-small cell obstructive lung cancer. Lung Cancer .2006;51: 225-236
8- Firuz Celikoglu, Seyhan I. Celikoglu, Eugene P. Goldberg. “Bronchoscopic intratumoral chemotherapy of lung cancer”
Lung Cancer (2008) 61, 1—12
9- Seyhan I. Celikoglu, MD,* Firuz Celikoglu, MD,* and Eugene P. Goldberg .”Intratumoral Cancer Chemotherapy Through a Flexible Bronchoscope” J Bronchol 11, Number 4, October 2004
10- Firuz Celikoglu, Seyhan I. Celikoglu and Eugene P. Goldberg. “ Intratumoural chemotherapy of lung cancer for diagnosis and treatment of draining lymph node metastasis.” Journal of Pharmacy and Pharmacology 2010; 62: 287–295
11- Firuz Celikoglu, MD,* Seyhan I. Celikoglu, MD,*and Eugene P. Goldberg, “Endobronchial Intratumoral Chemotherapy”
J Bronchol _ Volume 15, Number 4, October 2008
12- Firuz Çelikoğlu, Çiğdem Papilla , Seyhan Çelikoğlu.”Endobronşiyal İntratumoral Kemoterapi (ITK) nin Teknik Özellikleri” Solunum 2007; Vol: 9 Say›: 3 Sayfa: 175- 82
13- Firuz ÇELİKOĞLU, Çiğdem PAPİLA, Seyhan İ. ÇELİKOĞLU.” Akciğer kanserinde sitotoksik ilaçların
tümör içine direkt enjeksiyonu ile uygulanan endobronşiyal kemoterapi. Tüberküloz ve Toraks Dergisi 2008; 56(3): 337-343
14- Wolfgang Hohenforst-Schmidt. Firuz Çelikoglu, Seyhan Celikoglu .”Intratumoral chemotherapy for lung cancer: re-challenge current targeted therapies. Drug Design, Development and Therapy 2013:7
15. Monga SPS, Wadleigh RW, et al. Endoscopic treatment of gastric cancer with intratumoral cisplatin/epinephrine injectable gel: a case report. Gastrointest Endosc. 1998;48:415–417.
16. Monga SPS, Wadleigh RW et al. Intratumoral therapy of cisplatin/epinephrine injectable gel for palliation in patients with obstructive esophageal cancer. Am J Clin Oncol. 2000;23:386–392.
17-. Ning S, Yu N, Brown DM, et al. Radiosensitization by intratumoral administration
of cisplatin in a sustained-release drug delivery system. Radiother Oncol. 1999;50:215–223